Prostate MRI Procedure
Our Urology team is led by Dr. Robert Bates, one of the region’s leading Urologists.
Please review the information on this page to better understand the Prostate MRI and US Fusion Guided Biopsy of the Prostate.

Dr. Bates, Urologist


WHAT IS IT AND WHY IS IT DONE?
A biopsy is a procedure that takes a sample of tissue for study. The most common reason is to look for cancer.
The prostate gland is part of the male reproductive system. It produces a fluid that makes up most of what’s in semen.
Using advanced biopsy equipment, the MRI combines with ultrasound images to identify specific areas for biopsy of the prostate. A prostate biopsy is done with a biopsy needle.
This needle can be placed more accurately to get samples for testing with the help of the combined images.
MRI and US Fusion Guided Biopsy of The Prostate
Getting Ready
MRI Procedure
- Get your bloodwork for creatinine level done within 30 days before your MRI appointment.
- The MRI will be done at least 1 week before your biopsy.
- The prostate MRI will be scheduled for 2 hours. You may need to come early for your creatinine bloodwork.
- Be sure to hydrate for 24 hours with extra fluids after your MRI.
- After the procedure, take your antibiotics as prescribed.
Fusion Biopsy Procedure
- Your urine may be tested to see if you have a urinary tract infection. If you have a urinary tract infection, your prostate biopsy may be postponed while you take antibiotics to clear the infection.
- Follow the instructions you get to stop taking medicines before the procedure that can put you at higher risk of bleeding. This includes medicines such as warfarin (Coumadin), clopidegrel (Plavix), iveroxaban (Xarelto), Aspirin, ibuprofen (Advil, Motrin), and certain herbal supplements. Talk about any blood thinners you take with your urologist. Take all other medicines as normal.
- You can have a light breakfast the day of the procedure.
- After the biopsy you will receive antibiotic instructions.
DURING THE PROCEDURE
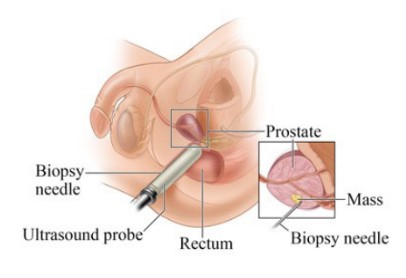
MRI/US fusion guided prostate biopsy is usually done in the outpatient procedure area. The MRI and ultrasound images help guide where the biopsy needle is placed. You’ll be asked to lie on your left side. The doctor will examine your prostate again. A lubricated ultrasound probe is then placed into your rectum. The ultrasound scan of your prostate is done. The doctor will see that image on the screen.
You may feel some discomfort or mild pain when the ultrasound probe is placed in your rectum. Local anesthesia (numbing medicine) is used to ease the discomfort. The biopsy (tissue sample) is taken using a needle and then sent to the lab for analysis.
AFTER THE PROCEDURE
Biopsy results should be available about 4 days after your procedure. The urology office will call you with your results.
After the procedure, it’s common to have rectal pain or discomfort for a few days. You may see blood in your urine, stool, or semen for up to 6 to 8 weeks. If you have pain, sit in a tub of warm water and take acetaminophen (Tylenol) as prescribed.
Avoid strenuous exercise and sex for 2 days after your biopsy, and then you may go back to your regular physical activities as your pain level allows.
Follow the instructions about activity and take pain medicine, if needed, as prescribed.
Go back to eating your regular diet after your biopsy, but avoid drinks with caffeine or alcohol, and don’t have spicy foods that may irritate the biopsy area.
Call your doctor or go to the Emergency Room if you have signs of infection such as:
- Fever greater than 38 °C
- Difficulty urinating
- Severe pain
- Heavy bleeding (more than a few drops or streaks)
PROSTATE MRI
COMMON QUESTIONS
Who should have this type of prostate biopsy?
This procedure is usually done if:
- You have a high or rising prostate-specific antigen (PSA) level.
- Your healthcare provider thinks that you may have prostate cancer.
- You’ve had an abnormal rectal exam.
- You’ve had abnormal findings on prostate MRI.
- Your genes put you at more risk to develop prostate problems.
- You’re being monitored for prostate cancer.
What are the benefits?
Some abnormal tissue growths (called tumors) that can grow in your prostate are clinically insignificant. This means that they don’t need any immediate treatment. They aren’t likely to pose a threat to your health.
Using the MRI image to guide your biopsy helps raise the chance of finding prostate tumors that need treatment. MRI images give precise information. This lowers the chance that a serious tumor will be missed, which can happen with a regular ultrasound biopsy.
This type of test causes less tissue damage. You’ll usually have a shorter recovery to get back to your daily activities.
What are the risks?
After this procedure you may have:
- Difficulty passing your urine – in rare cases, you may need a temporary urinary catheter.
- Bleeding in your stool, urine, and semen.
- Infection in the blood or urine.
Pain (usually very little). - Allergic reaction.
From Dr. Bates
I want to emphasize if there’s questions or concerns afterwards, no question is unreasonable to ask.
One of us is always available and we’ll get back to you. And if it’s something that we really need to see, we’ll make sure you get into the clinic as quickly as possible.
It’s a very straightforward procedure, very commonly done.
Caution: This material is not a substitute for the advice of a qualified health professional. This material is intended for general information only and is provided on an “as is”, “where is” basis. Although reasonable efforts were made to confirm the accuracy of the information, McKenzie Health does not make any representation or warranty, express, implied or statutory, as to the accuracy, reliability, completeness, applicability or fitness for a particular purpose of such information. McKenzie Health expressly disclaims all liability for the use of these materials, and for any claims, actions, demands or suits arising from such use.